
How Your Diet Can Affect Your Fertility
There are an abundance of factors that can affect a woman’s fertility. Female infertility can be the result of irregular ovulation, issues with the reproductive

There are an abundance of factors that can affect a woman’s fertility. Female infertility can be the result of irregular ovulation, issues with the reproductive

Over the years, endometrial ablation has become a fairly common procedure for women who experience irregular menstrual bleeding. It can be particularly helpful in cases

Here at Gynecology Associates of Gwinnett, there is no such thing as a small or silly question in regard to reproductive health and wellness. We

No woman should have to deal with the frustration and uncertainty brought on by irregular menstrual bleeding. In addition to being inconvenient, abnormal bleeding that
Here at Gynecology Associates of Gwinnett, we are passionate about being able to make meaningful connections with our patients. And there is no more important
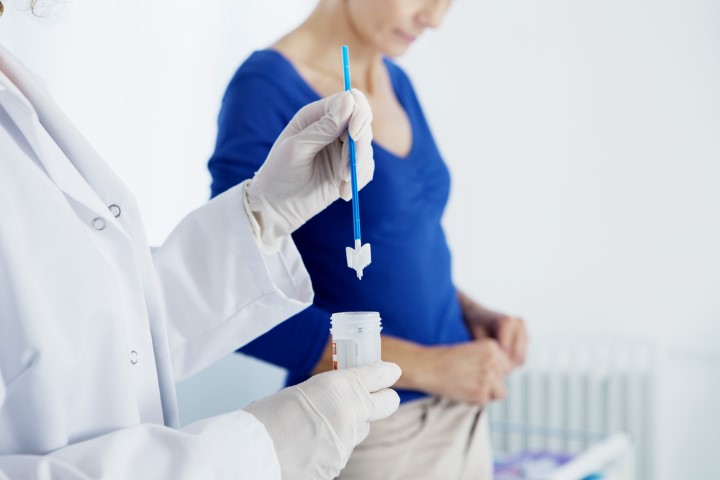
Undergoing a Pap smear, or Pap test is a common reason for a woman to request a visit with her gynecologist. A Pap smear is used as

Menopause is very complex and can affect every woman differently. However, there are some very common menopause symptoms that all women who transition into menopause should be
Menopause can affect a woman in many ways. Hormonal changes that the body experiences can have a profound impact on a woman’s health and wellness.

Urinary incontinence is a very common reproductive health concern for women of all ages. And while there are several different types of urinary incontinence, stress urinary incontinence

In recent years, more women than ever have undergone endometrial ablation to treat their irregular menstrual bleeding. Endometrial ablation uses radio frequency technology to burn/ablate the
Monday: 8:30AM–4:30PM
Tuesday: 8:30AM–4:30PM
Wednesday: 8:30AM–4:30PM
Thursday: 8:30AM–4:30PM
Friday: 8:30AM–12PM
Insurance & Self-Pay
Bill Pay